Treat antibiotics responsibly, guidance, education, tools (TARGET): antibiotic toolkit for primary care – Influence prescribers’ and patients’ personal attitudes, social norms and perceived barriers to optimal antibiotic prescribing used by the whole primary care team within the GP practice or out-of-hours setting.Make a personal pledge about action you’ll take to prevent infections and make better use of antibiotics. Antibiotic Guardian – A Public Health England campaign to encourage healthcare staff and patients to take action and slow antibiotic resistance.Antimicrobial prescribing and stewardship competencies – For all independent prescribers to help improve the quality of prescribing practice.Infection prevention and control commissioning toolkit – Royal College of Nursing guidance to support nursing staff and anyone involved in the commissioning or assurance of health and social care services.Guidelines for preventing healthcare-associated infections (Epic3) – Use these national evidence-based guidelines for preventing healthcare-associated infections.NICE guidelines: Prevention and control of healthcare-associated infections (pathway) – This pathway covers the prevention and control of healthcare-associated infections in primary, community and secondary care.Care Quality Commission: regulations for service providers and managers – safe care and treatment – The intention of this regulation is to prevent people from receiving unsafe care and treatment and prevent avoidable harm or risk of harm.WHO guidelines on hand hygiene in healthcare – Provides healthcare workers, hospital administrators and health authorities with a thorough review of evidence on hand hygiene in healthcare and specific recommendations to improve practices and reduce transmission of pathogenic microorganisms. 
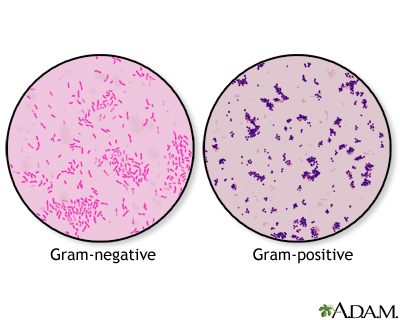
Guidance on the definition of healthcare associated Gram-negative bloodstream infections – The guidance explains, for the purposes of the NHS ambition to reduce healthcare-associated Gram-negative BSIs, how these infections will be defined according to where they are detected (community or hospital settings), and key healthcare-associated risk factors.Gram-negative blood stream infections: evidence and further resources. 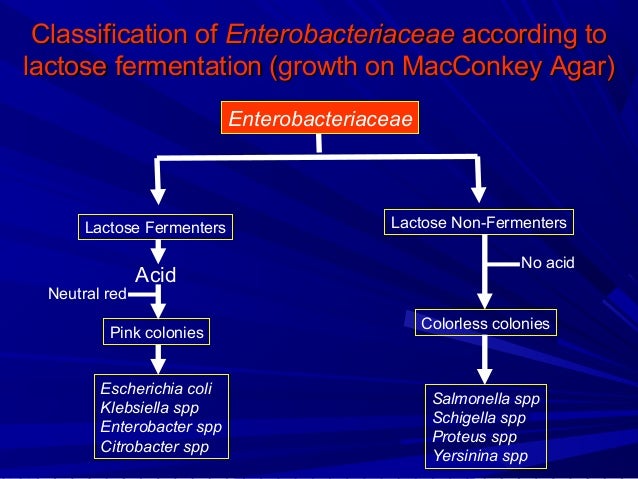
We would welcome any feedback on the content and utilisation of the tool by emailing the our IPC email address: collated a range of evidence, guidance, examples of practice and supportive resources into one place, providing easier access for health and social care workers leading on or interested in preventing Gram-negative bloodstream infections (GNBSI). It is also intended to assist organisations or systems to produce a focused and effective action plan for reducing E.coli BSIs. If you notice there are resources missing please let us know Gram-negative BSI system overview tool – This tool has been designed to allow organisations or systems to assess the overall approach to reducing E.coli blood stream infections (BSIs) and the engagement with the wider health economy in delivering a reduction. We recognise that effective prevention of infection is multifaceted and requires strong leadership, effective training programmes, and evidence-based guidelines and interventions. We’ve made suggestions rather than prescriptions about how to reduce these infections and pulled together a collection of tools for local teams. If you’d like to feedback on this resource, please email Tools for local teams coli BSIs occur before people are admitted to hospital, reduction requires a whole health economy approach. coli bloodstream infections because they represent 55% of all Gram-negative BSIs.Īs approximately three-quarters of E. We’re focusing on reducing healthcare associated E.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
